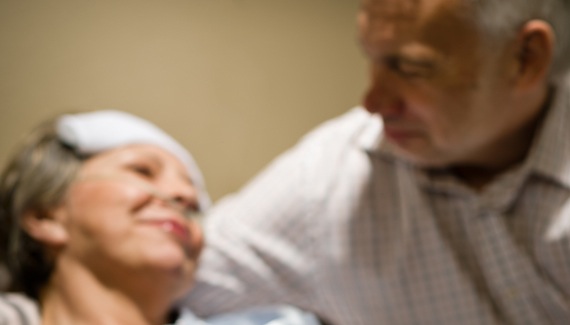
Canadians wants open and frank discussion about the issues surrounding death and dying.
That was the message the Canadian Medical Association heard repeatedly during a series of public town hall meetings held across Canada and involving several hundred people.
The results of this consultation, which also involved online and social media components, were released by the CMA in its report ‘End-of-life care: A national dialogue’.
“We set out to listen to what Canadians had to say on the important issues involved in care at the end-of-life and people demonstrated they were more than willing to reciprocate,” said CMA President Dr Louis Hugo Francescutti who attended all five meetings.
The report quotes a number of participants who cited accounts of excellent palliative and hospice care received across the country but also others documenting “horror stories” associated with poor end-of-life care received by relatives.
The report makes a number of conclusions based on the consultation, including the following:
All Canadians should to discuss end-of-life wishes with their families or other loved ones
Advance care directives should be prepared by all Canadians that are appropriate and binding for the jurisdiction in which they live
A national palliative care strategy is needed
All Canadians should have access to appropriate palliative care services
More education about palliative care approaches and services and knowledge about advance care directives is required for medical students, residents and practicing physicians
If the law in Canada is changed to allow euthanasia or physician-assisted dying, strict protocols and safeguards are required to protect vulnerable individuals and populations
Palliative care experts who spoke during the meetings stressed the importance of making comprehensive palliative care services available to everyone and noted that such care often “falls apart” outside major urban centres.
On the issue of advance care directives, the report states “there was almost universal agreement about the importance of advance care directives and the need for people to have discussions with family members and loved ones about their wishes for end-of-life care at various stages throughout their life.”
“While it was clear members of the public often had diametrically opposed views on the controversial topic of euthanasia and physician-assisted dying, common ground was evident on many other important issues ranging from the importance of advance care directives to the need for a comprehensive palliative care strategy in Canada,” the report noted.
“People understand the importance of discussing death and dying and are eager for more information and resources to help support these discussions,” Francescutti said.
“With Bill 52 in Quebec and the Supreme Court of Canada ruling on a case involving physician-assisted dying this fall, this report could not be more timely,” he said.
“The conclusions from the report will guide not only the CMA in its own deliberations at its annual General Council meeting in August but also, I hope, politicians and policy makers who have an obligation to listen to what Canadians have to say on these issues.”
The report was released on the same day that the CMA applied to intervene in the Supreme Court hearing on physician assisted dying, as a friend of the court, to seek to have the information heard during the town halls considered.
Canadajournal/Press Releases
 Canada Journal – News of the World Articles and videos to bring you the biggest Canadian news stories from across the country every day
Canada Journal – News of the World Articles and videos to bring you the biggest Canadian news stories from across the country every day