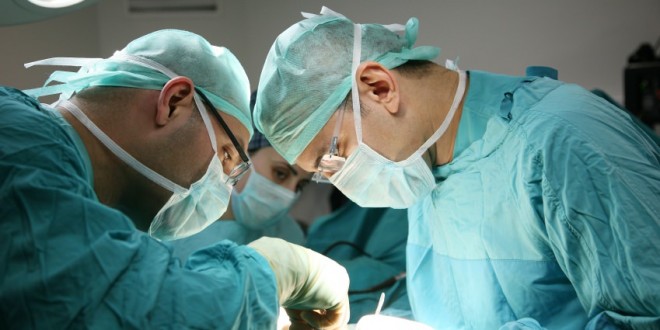
Now that they are living longer, solid organ transplant recipients (SOTRs) face an increased risk of dying from cancer.
The study published today in JAMA Oncology examined health records of 11,061 patients who had solid organ transplants in Ontario between 1991 and 2010. Solid organ transplants involve organs such as the heart, liver, lungs or kidneys, but not hollow organs such as intestines or non-solid tissues like bone marrow or blood.
Senior author Dr. Nancy Baxter, a colorectal surgeon at St. Michael’s Hospital and senior scientist at the Institute for Clinical Evaluative Sciences, said the study found nearly one-fifth of the deaths in this group were cancer-related: a rate nearly three times that of the non-transplant population.
Children with organ transplants had higher rates of cancer-related death when compared to the general transplant group. The risk was lower for patients over the age of 60; however cancer-related deaths were still much higher among this population.
When patients with pre-transplant cancers were excluded, the overall mortality rate was still twice as high when compared with the general population. Once a malignancy was diagnosed, transplant recipients were less likely to survive than non-transplant cancer patients.
“We know that solid organ transplant recipients have an increased incidence of malignancy after transplantation compared to the general population,” said Dr. Baxter. “But until now, studies have not separated deaths caused by recurrent pre-transplantation malignancies from deaths caused by new malignancies.”
Two-thirds of the cancer-related deaths in the study were linked to new malignant tumours or growths that appeared after a transplant. Skin cancer carried the highest risk of death – at 30 times higher in transplant recipients – followed by liver cancer and Non-Hodgkin’s Lymphoma.
“There are many explanations for the increased cancer mortality seen in this population,” said Dr. Sergio Acuna, the study’s lead author and a postdoctorate student in clinical epidemiology and health care research at the University of Toronto and St. Michael’s. “For example, the immunosuppression needed for patients to not reject their transplanted organ enables cancers to take hold more aggressively. Further, once a malignancy is diagnosed, these patients may receive less aggressive cancer treatment because they have additional illnesses, as well as fears that transplant rejection may occur.”
The researchers noted that cancer incidence is expected to grow within this population over the next decade as the age of transplant recipients rises with improved survival post-transplant lengthening patient exposure to immunosuppression.
Transplant patients receive cancer screening and prevention recommendations similar to those for the general population, but the group’s significantly increased risk calls for a more targeted approach, the authors said.
“We suggest that ongoing screening strategies be more closely targeted to a patient’s history and specific cancer risk,” said Dr. Baxter. “Since the risk of death from cancer is very high for this population, we also recommend that health care providers counsel these patients to take every possible precaution to reduce their risk, including limiting sun exposure, quitting smoking, reducing alcohol consumption, improving diet and increasing physical activity.”
Agencies/Canadajournal
 Canada Journal – News of the World Articles and videos to bring you the biggest Canadian news stories from across the country every day
Canada Journal – News of the World Articles and videos to bring you the biggest Canadian news stories from across the country every day