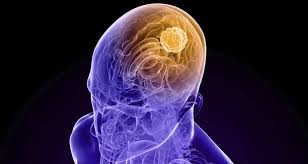
A new study has explained why brain tumors occurred more often in males and regularly are more damaging than similar tumors in females.
The new research at Washington University School of Medicine in St. Louis recognized that retinoblastoma protein (RB), a protein known to lessen cancer risk, is significantly less active in male brain cells than in female brain cells.
“This is the first time anyone ever has identified a sex-linked difference that affects tumor risk and is intrinsic to cells, and that’s very exciting,” said senior author Joshua Rubin, MD, PhD. “These results suggest we need to go back and look at multiple pathways linked to cancer, checking for sex differences. Sex-based distinctions at the level of the cell may not only influence cancer risk but also the effectiveness of treatments.”
Rubin noted that RB is the target of drugs now being evaluated in clinical trials. Trial organizers hope the drugs trigger the protein’s anti-tumor effects and help cancer patients survive longer.
“In clinical trials, we typically examine data from male and female patients together, and that could be masking positive or negative responses that are limited to one sex,” said Rubin, who is an associate professor of pediatrics, neurology and anatomy and neurobiology. “At the very least, we should think about analyzing data for males and females separately in clinical trials.”
Scientists have identified many sex-linked diseases that either occur at different rates in males and females or cause different symptoms based on sex. These distinctions often are linked to sex hormones, which create and maintain many but not all of the biological differences between the sexes.
However, Rubin and his colleagues knew that sex hormones could not account for the differences in brain tumor risk.
“Male brain tumor risk remains higher throughout life despite major age-linked shifts in sex hormone production in males and females,” he said. “If the sex hormones were causing this effect, we’d see major changes in the relative rates of brain tumors in males and females at puberty. But they don’t happen then or later in life when menopause changes female sex hormone production.”
Rubin used a cell model of glioblastoma to prove it is easier to make male brain cells become tumors. After a series of genetic alterations and exposure to a growth factor, male brain cells became cancerous faster and more often than female brain cells.
In experiments designed to identify the reasons for the differences in the male and female cells, the team evaluated three genes to see if they were naturally less active in male brain cells. The genes they studied — neurofibromin, p53 and RB — normally suppress cell division and cell survival. They are mutated and disabled in many cancers.
The scientists found RB was more likely to be inactivated in male brain cells than in female brain cells. When they disabled the RB protein in female brain cells, the cells were equally susceptible to becoming cancers.
“There are other types of tumors that occur at different rates based on sex, such as some liver cancers, which occur more often in males,” Rubin said. “Knowing more about why cancer rates differ between males and females will help us understand basic mechanisms in cancer, seek more effective therapies and perform more informative clinical trials.”
Agencies/Canadajournal
 Canada Journal – News of the World Articles and videos to bring you the biggest Canadian news stories from across the country every day
Canada Journal – News of the World Articles and videos to bring you the biggest Canadian news stories from across the country every day